Skin and Pigment Theory
3 hours estimated · 7 sections
SKIN IS NOT A CANVAS.
SKIN IS A FILTER.
KORT TEACHES YOU TO WORK WITH THE FILTER, NOT AGAINST IT.
Every impression you place passes through the client's unique biological system — their melanin, their healing response, their skin chemistry. The pigment you deposit is not the colour the client will see. Understanding this transformation is the difference between predictable results and colour surprises.
MODULE OVERVIEW
Modules 1 and 2 taught you to read the skull and plan density. Module 3 teaches you what happens when pigment meets skin — why the same pigment looks different in different skin types, why all SMP shifts cool during healing, and why Fitzpatrick IV–VI skin requires a fundamentally different approach than lighter skin tones.
Skin is not a passive canvas. It is an active biological system that filters, modifies, and challenges every pigment you deposit. The epidermis is a translucent layer that sits above your work and affects how light reaches and returns from the pigment. The dermis is a dynamic tissue that can accept, reject, encapsulate, or migrate the particles you place. And melanin — the pigment already in the client's skin — acts as a colour filter that transforms every deposit before the observer's eye sees it.
This module gives you the structural understanding you need to predict and control these interactions.
The pigment you place is not the colour the client will see. Every impression passes through the client's epidermis twice — once on the way in (light), once on the way out (reflected light). Melanin filters both passes. Understanding this transformation is what separates predictable results from colour surprises.
Scalp Skin Structure
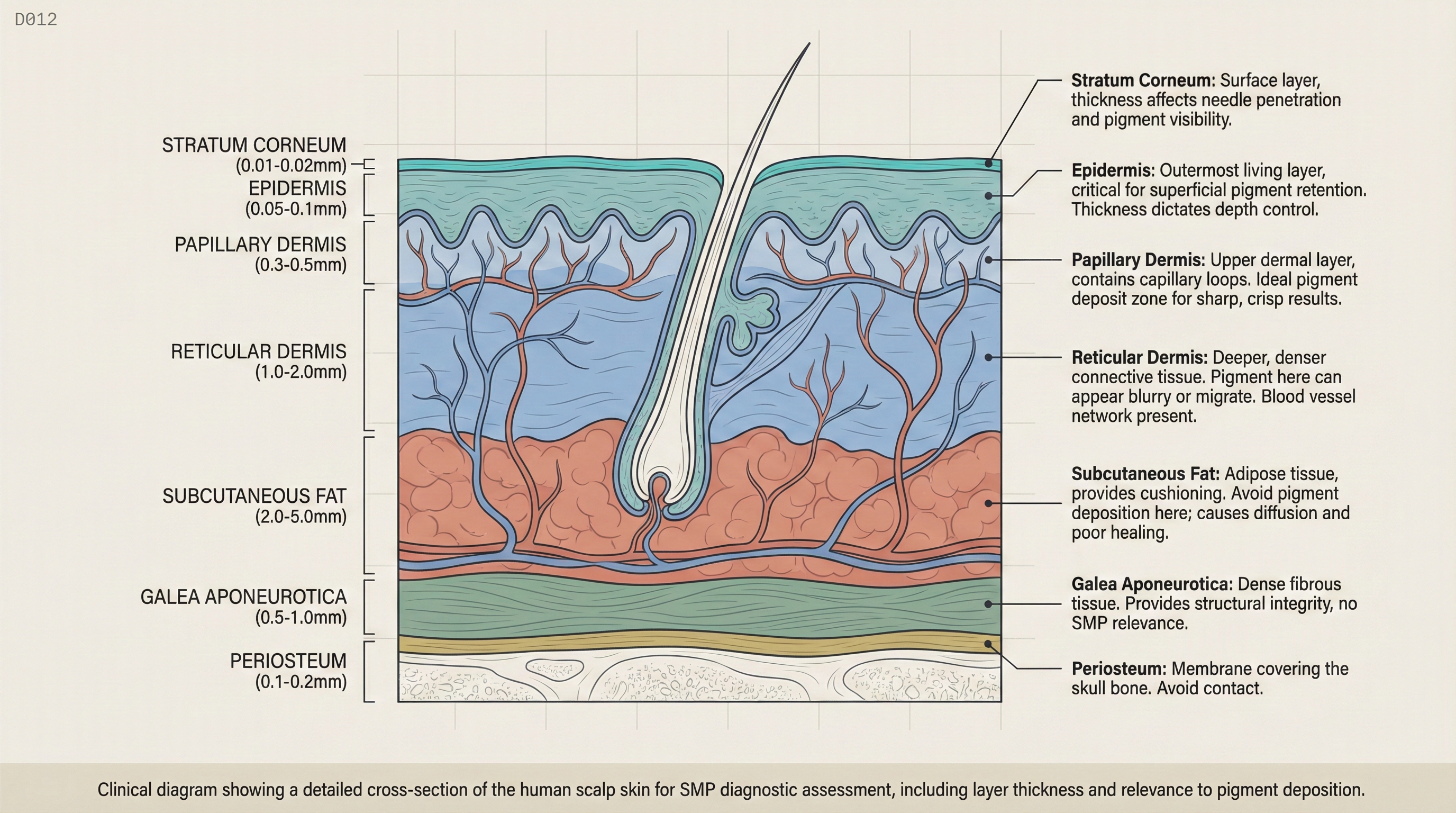
The scalp is not uniform skin. It has distinct layers, and understanding where your pigment needs to land — and where it must not land — is the foundation of consistent SMP results.
The Three Primary Layers
Epidermis (The Surface)
The outermost layer, approximately 0.1mm thick on the scalp. The epidermis is avascular (no blood supply) and constantly renewing through cell turnover. Pigment deposited in the epidermis will shed within days to weeks as the epidermal cells migrate to the surface and slough off. This is why epidermal-only deposits (too shallow) fade rapidly.
The epidermis also contains melanocytes — the cells that produce melanin. On Fitzpatrick IV–VI skin, the epidermal melanin concentration is high enough to act as a significant colour filter for any pigment deposited below it.
Dermis (The Target)
The layer beneath the epidermis, approximately 1–2mm thick. The dermis contains collagen fibres, blood vessels, sebaceous glands, and hair follicles. It is divided into two regions with different SMP implications.
Upper dermis (~0.5mm): The target zone. Collagen fibres here are tightly packed, which holds pigment particles in defined clusters. Impressions placed in the upper dermis retain their shape, remain distinct, and heal as clean, defined points or strokes. This is where every KORT impression should land.
Mid to lower dermis (1.0mm+): Danger zone. Collagen fibres are looser. Blood supply is richer. Subcutaneous fat begins to interface. Pigment deposited here migrates laterally, following the path of least resistance through loose connective tissue and fat. The result is the blowout: impressions that start as defined dots and heal as diffuse, blurry patches.
Hypodermis (The Danger)
The deepest layer, primarily fat cells and large blood vessels. No SMP pigment should ever reach the hypodermis. If it does, the pigment disperses unpredictably through adipose tissue, creating deep discolouration that is extremely difficult to correct. Hypodermis deposits also carry higher infection risk due to the vascular density.
The scalp does not have a uniform number of layers everywhere. At the vertex and crown, the scalp has three primary layers with relatively thin total thickness. At the temporal and occipital regions, additional fascial layers increase total thickness to five layers. This means your depth target is the same (upper dermis, ~0.5mm) but the margin for error is different. At the vertex, you are closer to the hypodermis if you go too deep. This is why vertex treatments require the most precise depth control — and why blowouts are most common at the crown.
Ready to test your knowledge?
Complete the module quiz to track your progress. You need 80% to pass.
Start Quiz (10 questions)